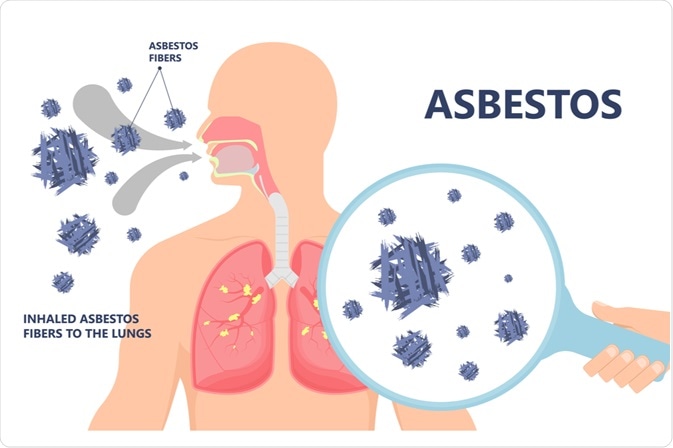
Mesothelioma is a type of cancer that begins in the epithelial cells usually found on the outside of the lungs. Mesothelioma can begin anywhere where epithelial cells are normally located, although the most common site is the parietal pleura. Another name for mesothelioma is malignant mesothelioma.
Mesothelioma is associated with asbestos exposure in most, but not all, cases. Many patients exposed to asbestos will also have areas where the pleura has become abnormally thickened. These areas are called pleural plaques and can usually be seen on imaging of the lungs (X-ray or CT scan). When examined under a microscope, pleural plaques consist of dense collagen layers that can have the appearance of basket weave.
Lungs and pleura
Your lungs are located inside your chest in a space known as the pleural cavity, or pleural space. The surface of your lungs and chest wall is covered by a thin type of tissue called the pleura (singular pleura ) . The pleura that covers the lung is called the visceral pleura and the pleura that covers the chest wall is known as the parietal pleura. Two layers of pleura can be understood as a balloon within a balloon. The inner (visceral) pleura is separated from the outer (parietal) pleura by a thin space called the pleural cavity.
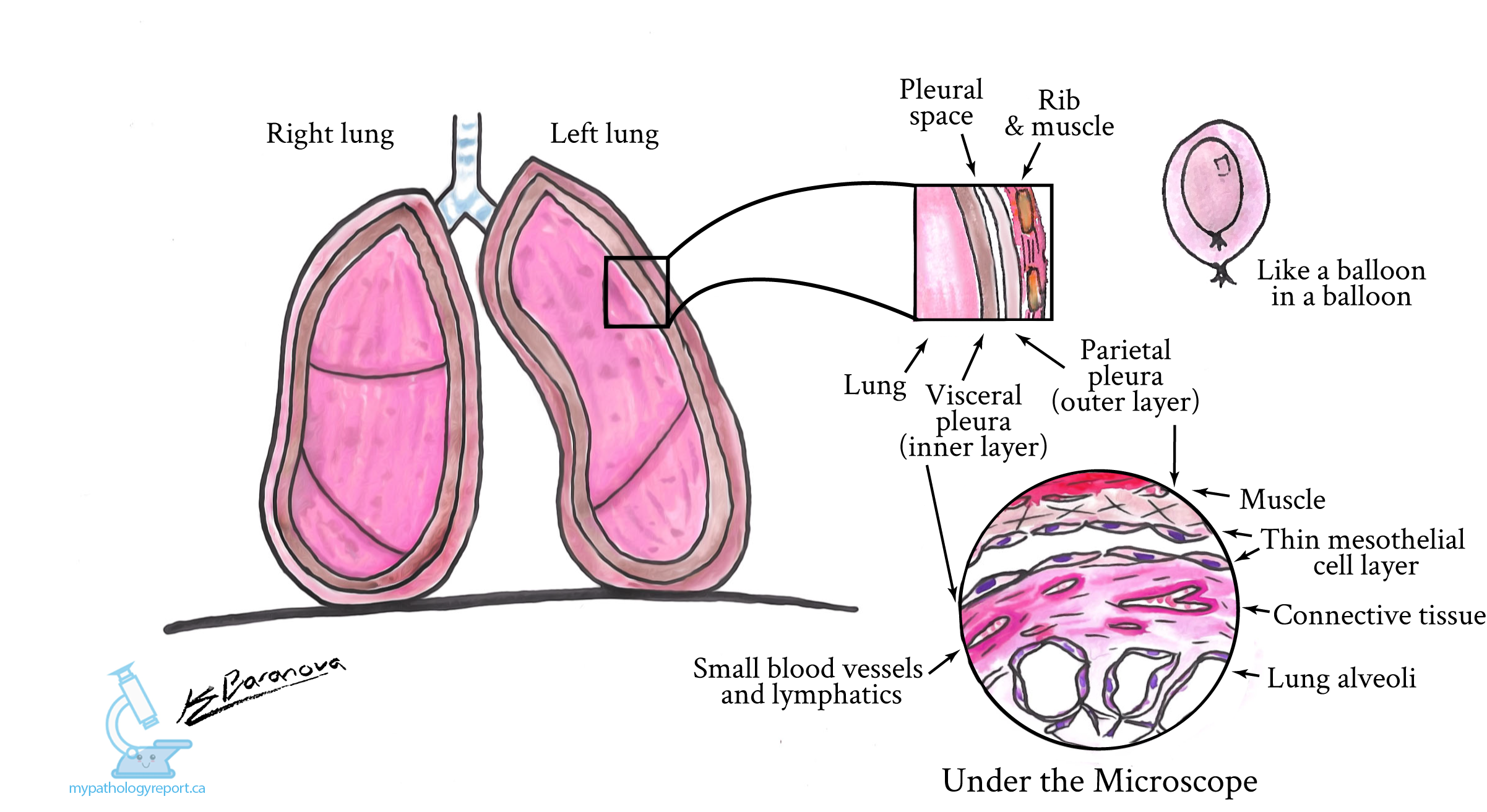
Pathologists call the pleural cavity a potential space because it is not usually filled with air. Under normal conditions, there is a thin layer of fluid between the two layers of the pleura. Under the microscope, the pleura is made up of a layer of cells called epithelial cells . These cells are small, flat to cuboid, with well-defined cellular boundaries. The part of the cell that contains the cell’s genetic material, the nucleus , usually found in the center of the cell.
How do pathologists make this diagnosis?
Mesothelioma is usually diagnosed after a small sample of tissue is removed in a procedure called a biopsy . In some cases, additional surgery may be performed. Diagnosing mesothelioma can be difficult because noncancerous conditions such as infection or pleural effusion can lead to changes in epithelial cells that can look similar to cancer under a microscope. In order to diagnose mesothelioma, your pathologist needs to see the epithelial cells that make up a tumor, or that has spread beyond the pleura to surrounding tissues or the lungs. The proliferation of epithelial cells into surrounding tissues is called invasion .
When examined under a microscope, other types of cancer can look very similar to mesothelioma. Most pathologists will perform a test called immunohistochemistry to help them determine whether the abnormal cells are phenotypes or cells from another part of the body.
When immunohistochemistry is performed, epithelial cells will typically show the following results:
- WT-1 – Positive
- Calretinin – Positive
- D2-40 – Positive
- Cytokeratin 5/6 – Positive
- MOC-31 – Negation
- BerEP4 – Negation
- Polygonal CEA – Negative
- TTF-1 – Negation
Pathologists usually need a combination of immunohistochemical tests to help them determine whether the abnormal cells are mesothelial cells or whether they are from another part of the body.
To differentiate mesothelioma from other conditions, some pathologists may use other immunohistochemical tests including BAP1 and mTAP. Both of these proteins are found naturally in tissues throughout the body. However, it does not usually appear in mesothelioma. For this reason, a negative result for BAP1 or mTAP supports the diagnosis of mesothelioma.
Surgery to remove the tumor
You may see the name of the surgical procedure on your pathology report. The name of the procedure depends on the amount of tissue removed.
Types of procedures include:
- Extrapleural pneumonectomy – This procedure involves removing the lung, the pericardium (the membrane that covers the heart), part of the diaphragm, and the parietal pleura.
- Extended pleurectomy/removal – this procedure involves removal of the visceral and parietal pleura with excision of the pericardium (the membrane that covers the heart) and the septal hemisphere.
- Pleurectomy/removal – this procedure involves removing the visceral and parietal pleura.
- Partial pleurectomy – This procedure involves removing part of the pleura tissue.
tissue type
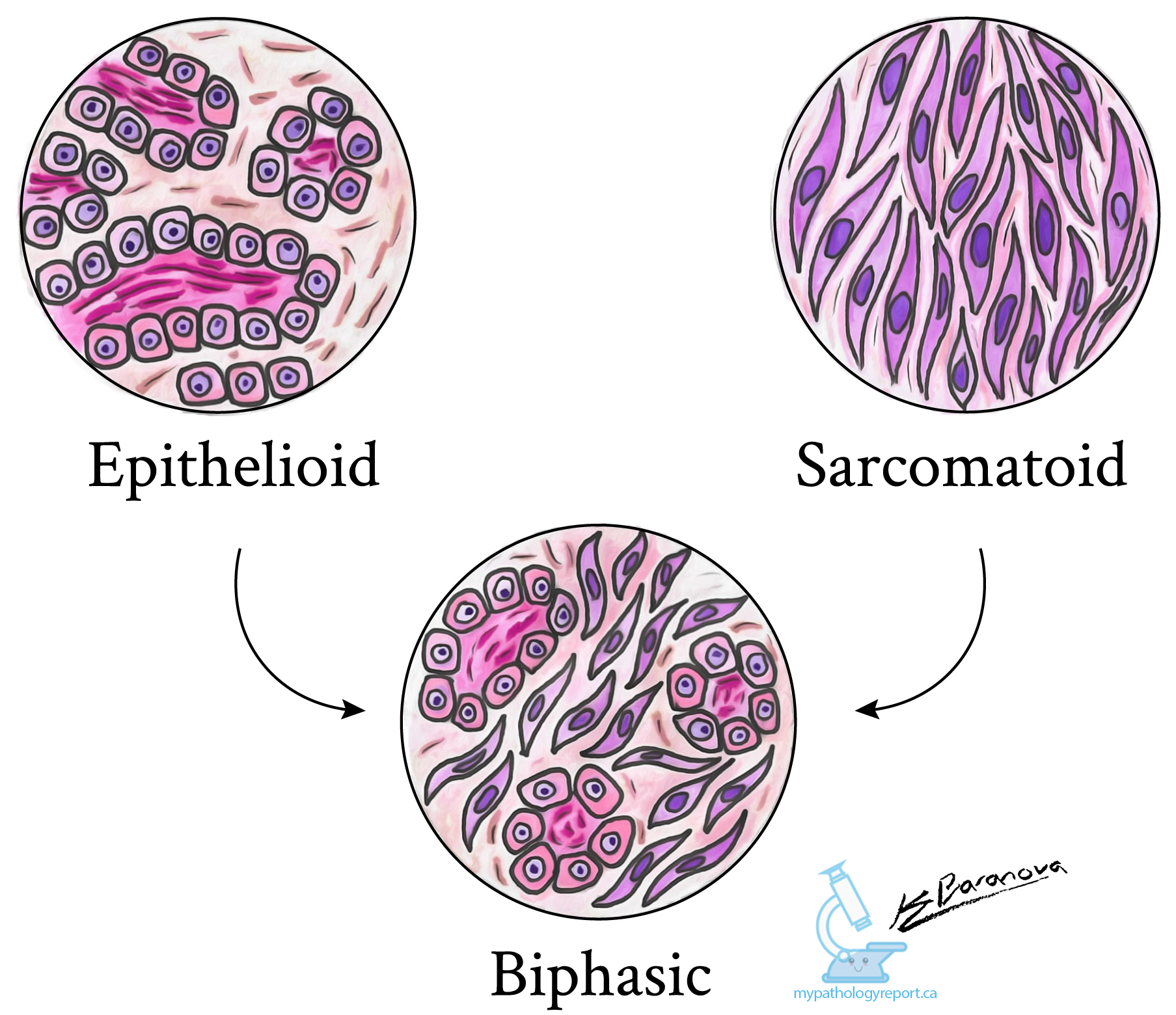
There are three types of mesothelioma that depend on the shape of the cells when examined under a microscope. Pathologists decide the type by looking at the size and shape of the cells and the way the cells stick together.
- Mesothelioma – this type consists of small cells of oval to cuboid shapes that join together, often forming small tubular or papillary structures.
- Sarcomatoid mesothelioma – this type consists of cells that are longer than they are wide. Pathologists describe these cells as spindle cells . In contrast to cells in epithelial-type mesothelioma, spindle cells also do not stick together to form structures and spread widely into surrounding tissues.
- Biphasic mesothelioma – this type consists of a mixture of epithelial-like and sarcomatoid cells. To be called biphasic, your pathologist needs to see at least 10% of each cell type in tissue samples examined under a microscope.
Desmoplastic mesothelioma is another type of mesothelioma that is related to the sarcomatoid type. Diagnosing mesothelioma can be difficult for a pathologist. The tumor consists of dense fibrous tissue with abnormal spindle cells.
The histological type is important because patients with the epithelial type will usually have the best references followed by biphasic and then sarcomatoid. The histological subtype may affect the surgical procedures or therapies used to treat the specific type of mesothelioma.
The number of tumors
Most mesotheliomas grow as a single large tumor that covers both the parietal and visceral pleura. It is often difficult to determine where the tumor stops and where a normal, healthy pleural begins. However, some mesotheliomas grow as a smaller tumor that is easier to separate from the surrounding healthy normal pleura. Pathologists describe these tumors as mesothelioma. Patients with localized mesothelioma have the best references and may be able to undergo lumpectomy successfully.
margins
A margin is the normal tissue that surrounds the tumor and is removed along with the tumor at the time of surgery. If you have had a complete resection with extrapleural pneumonectomy, the pathologist will look for cancer cells at the cut edge of the tissue.
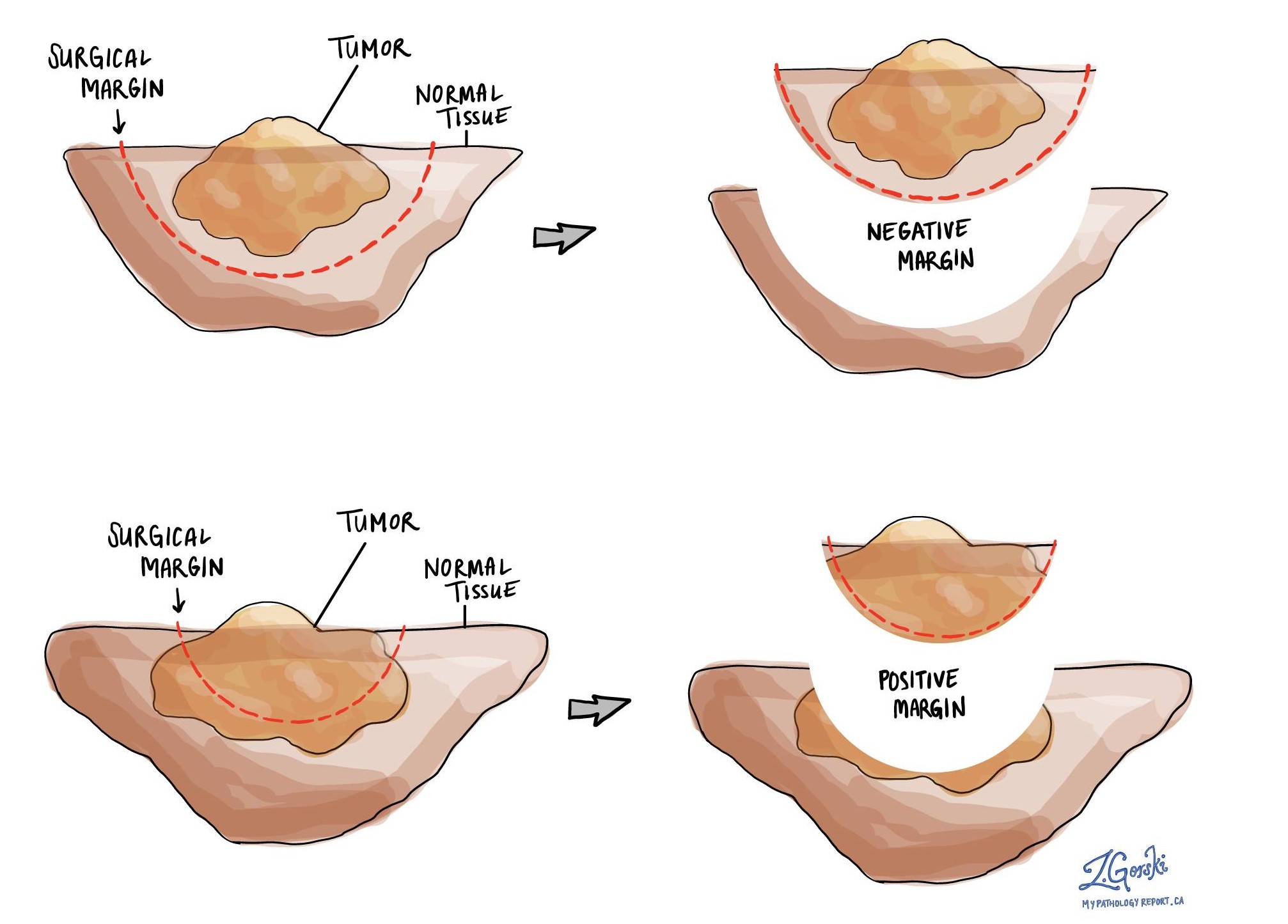
If no neoplastic cells appear at the cut edge of the tissue, the margin is called negative. If cancer cells are seen on the edge of the cut tissue, the edge is called positive. A positive margin is important because it is associated with a higher risk that the tumor will return in the same site (local recurrence) after treatment.
treatment effect
Some patients will receive chemotherapy or radiotherapy before the tumor is surgically removed. If you received chemotherapy or radiotherapy before surgery, your pathologist will examine the tumor under a microscope to see how much of the tumor is still alive (viable). This is called treatment effect.
To determine the effect of treatment, the pathologist will measure the amount of the tumor that is live (viable) and divide this number by the amount of the total tumor. The effect of treatment is usually described as greater or less than 50% of the remaining viable tumor.
How well the tumor responds to treatment may help your oncologist understand how well the tumor is being treated with chemotherapy and can be used to help guide further treatment.
lymph nodes
Lymph nodes are small immune systems scattered throughout the body. Cancer cells can travel from a tumor to a lymph node through lymph ducts in and around the tumor. The movement of cancer cells from a tumor to a lymph node is called a lymph node metastasis
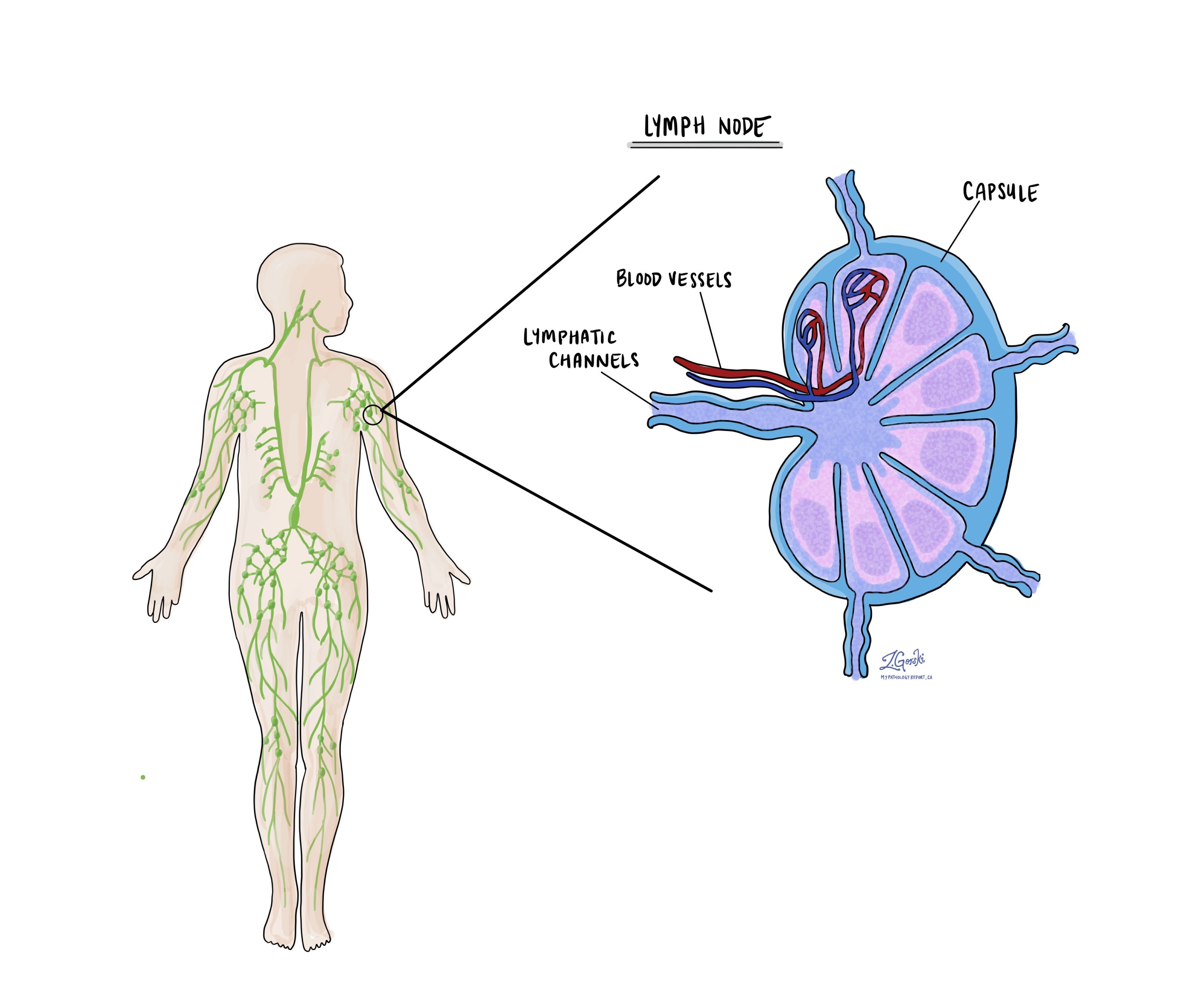
Lymph nodes from the neck, chest, and lungs can be removed at the same time as the tumor is removed. The pathology report will describe the number of lymph nodes examined. A pathologist will carefully examine each lymph node for cancer cells. Lymph nodes that contain cancer cells are called positive while lymph nodes that do not contain any cancer cells are called negative.
The finding of tumor cells in the lymph node increases the nodal stage (see pathological stage below) and correlates with deterioration refs. The nodal stage depends on where the lymph node is located with the cancer cells.
- pathological stage
Pathological staging of mesothelioma is based on the TNM staging system, an internationally recognized system originally established by the US Joint Commission on Cancer This system uses information about the primary tumor (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathological stage (pTNM). Your pathologist will examine the tissue provided and give each part a number. In general, a higher number means more advanced disease and worse references
Tumor stage (pT) for mesothelioma
Mesothelioma is given a tumor stage between 1 and 4 based on invasion by the tumor into other structures and tumor resection (ability to surgically remove).

Nodal stage (PN) of mesothelioma
Mesothelioma is given a nodal stage between 0 and 2 based on the presence or absence of precancerous cells in a lymph nodes the location of the lymph nodes that contain precancerous cells.
- NX – lymph nodes were not sent for pathological examination.
- N0 – No cancer cells were found in any of the lymph nodes examined
- N1 – Cancer cells are found in at least one lymph node of the hilum or mediastinum of the same side as the tumor.
- N2 – cancer cells are found in at least one lymph node of the opposite side of the mediastinum or outside the chest.
Metastatic stage (pM) of mesothelioma
Mesothelioma is given a metastatic stage of 0 or 1 based on the presence of the cancer at a distant site in the body (for example, the brain). The metastatic stage can only be determined if tissue is sent from a remote site for pathological examination. As this tissue is rare, the metastatic stage cannot be determined and is listed as pMX.